4 min read
771 words
If you come to this post via Google then you already know what Endometrial Ablation is. For those who don’t know it is a procedure to remove a thin layer of tissue in the uterus. One in seven women experience abnormal uterine bleeding during their reproductive years, as noted by Fraser et al. Endometrial ablation has emerged as a widely favored surgical option among gynecologists to address this issue. In this blog post, I will recount my experience with endometrial ablation.
My experience with endometrial ablation
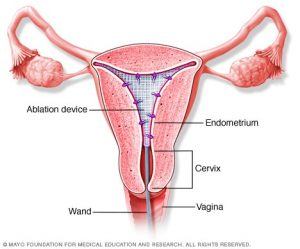
I commenced my journey with a detailed consultation with my gynecologist. During this meeting, my physician clarified that endometrial ablation is a minimally invasive technique aimed at eliminating the uterine lining (endometrium) to alleviate or cease menstrual bleeding.
For numerous women, including myself, this procedure presents an opportunity to regain autonomy over their bodies and enhance their overall quality of life. Having exhausted all available medications and non-surgical options, I was enthusiastic to learn about this potential solution.
After going over my medical history and lifestyle with my doctor, we both felt confident that I was a good candidate for the procedure. It was comforting to learn that endometrial ablation is usually suggested for women who have finished having children, as it can impact future fertility. Since I have achieved my family goals, I experienced a wave of relief, realizing that this might be the solution I had been seeking.
What They Don’t Tell You
At the age of 27, I had my first endometrial ablation to address my heavy menstrual bleeding. Having decided that my family was complete and with my husband having undergone a vasectomy, my gynecologist recommended this procedure.
After the first attempt didn’t yield the desired results, I underwent a second procedure two years later, which proved to be completely effective in alleviating my heavy periods—so much so that they ceased entirely.
However, my body continued to respond hormonally. With my ovaries still active, I experienced the natural cycle of ovulation, which persisted for over 15 years.
This led to complications such as endometrial regrowth, an excessive buildup of uterine lining, the formation of uterine polyps, and chronic pelvic pain. Over a span of six years, I consulted three different gynecologists before one suggested a biopsy, suspecting the possibility of endometrial cancer.
Unfortunately, my gynecologist faced challenges in performing a successful biopsy due to scarring in the uterus. Given the risk of missing cancer behind the adhesions, a complete hysterectomy was recommended. Thankfully, the surgery went well, and no cancer was detected. I consider myself fortunate, and my heart goes out to those who face the harsh reality of undiagnosed cancer.
My experience, along with others, highlights the ongoing challenges in accurately evaluating the endometrial cavity after an ablation procedure.
Why does endometrial ablation fail
At first glance, it might seem completely harmless. However, the issue arises years later when uterine scarring can develop.
The age at which you undergo this procedure is the most critical risk factor. Women who have Endometrial Ablation before turning 40 face a notably higher risk of needing a hysterectomy. In fact, case studies indicate that for those under 40, the hysterectomy rate reaches 40%.
Endometrial ablation isn’t a sterilization technique.
Endometrial ablation does not serve as a form of contraception. It is still possible to become pregnant afterward, but such pregnancies carry increased risks. The damage to the uterine lining may lead to a higher chance of miscarriage, or there is a possibility of an ectopic pregnancy occurring.
Closing thoughts
I can’t advise you against considering an Endometrial Ablation; that decision ultimately rests with you. I’m also not in a position to propose an alternative. My aim here is to share my experience with endometrial ablation, hoping to provide you with a different perspective on this procedure.
By recounting my experience with endometrial ablation, I hope to spark a dialogue. I wouldn’t wish my experience on anyone. Every individual’s path is distinct, and it’s crucial to evaluate your choices thoughtfully. I urge you to reflect deeply on your decisions, as your health and well-being are of paramount importance.
Works Cited
Challenges of endometrial evaluation in women with postmenopausal bleeding with history of ablation – case series
https://www.ejog.org/article/S0301-2115(16)30465-1/fulltext
Long-Term Complications of Minimally Invasive Endometrial Ablation Devices
https://www.liebertpub.com/doi/10.1089/gyn.2009.0016
Can anything be done to prevent pregnancy after endometrial ablation?
https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/1471-0528.14853
Post ablation risk factors for pain and subsequent hysterectomy.
https://www.ncbi.nlm.nih.gov/pubmed/25437717
Likelihood of Hysterectomy after Endometrial Ablation
https://www.reliasmedia.com/articles/112729-likelihood-of-hysterectomy-after-endometrial-ablation
I’m sorry you had a bad experience.
I’m grateful you took the time to share your thoughts on endometrial ablation. Negative experiences are often overlooked in discussions, but they can provide critical information for those weighing their options