6 min read
1048 words
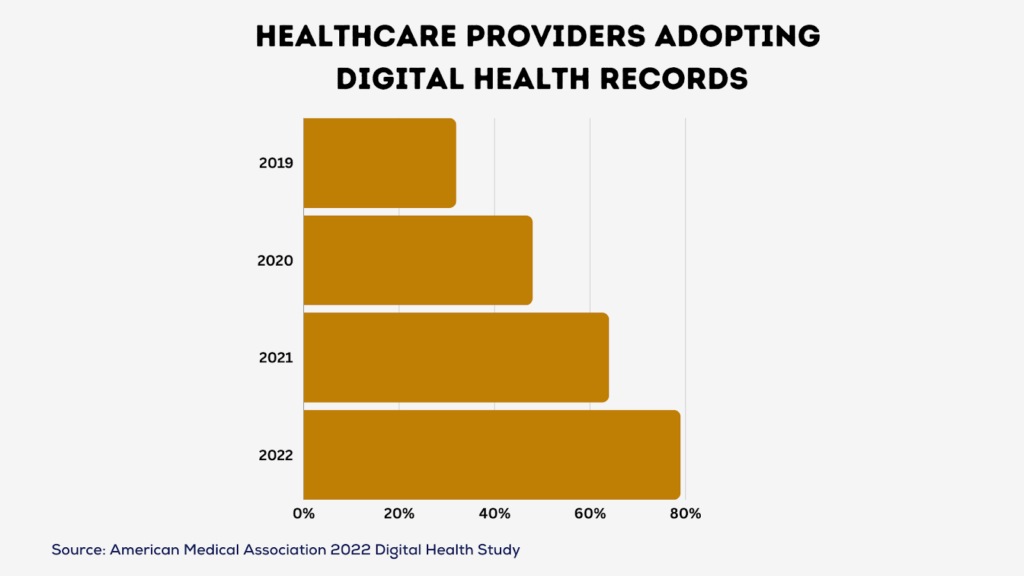
The healthcare landscape is rapidly adopting digital health records to improve efficiency and enhance patient outcomes. Nowhere is this more evident than in the realm of nutritional care. Digital health records are revolutionizing nutrition management for chronic diseases like Type 2 Diabetes, facilitating personalized nutrition plans tailored to each patient.
Digital health records significantly improve patient nutrition tracking. They excel in managing diets for conditions such as diabetes. Records now connect food details directly to medical care.

How Do Digital Health Records Help?
Digital health records now enable doctors to efficiently monitor various aspects of patient dietary information, including calories, nutrients, meal times, food restrictions, and more. The difference between EHR and EMR is crucial in this context. While EMRs are limited to a single healthcare provider, EHRs are accessible across different health organizations. This digitized information is readily accessible and significantly reduces the time doctors need to spend on record-keeping.
By connecting this information directly to medical records in one place, care teams get a comprehensive view of someone’s health for better coordination.
Now emerging innovations focus on tailored meal planning. Systems can take an individual’s health history and integrate it with their real-time nutrition monitoring. This way the technology can design hyper-personalized dietary recommendations that meet both medical needs and personal preferences perfectly.
The more specific to someone’s unique health markers and tastes a nutrition plan is, the more effective it becomes. The future of digital health aims to use advanced analytics to map individuals’ changing health metrics to food suggestions calibrated just for them. Such true personalization promises to improve adherence, health outcomes, and patient satisfaction.
Using Tech for Better Digital Health Records
Wearable technology like smartwatches and fitness trackers adds key real-time health data. When paired with digital diet monitoring, they give complete nutritional insights. Doctors get a clear picture to personalize meal plans. Patients stay motivated by watching their progress.
Wearables Track Vital Signs
Fitness bands and watches measure:
- Heart rate patterns
- Blood pressure trends
- Oxygen saturation levels
- Breathing rates
These vital signs reflect nutritional status indicators such as fluid/electrolyte balance. Changes may signal deficient micronutrient intake.
Activity Level Insights
Steps per day, movement times, and calorie burns from exercise track patient activity. Increasing movement requires upping energy foods. Drops may indicate illness or poor diet discipline.
Sleep Cycle Analysis
Not sleeping well negatively impacts appetite hormones and metabolism. Light versus deep sleep data guides nutrition adjustments to optimize rest.
Location-Based Logging
GPS functionalities in smart devices pinpoint eating at restaurants frequently. This clues into excess sodium or sugar intake hindering nutrition goals.The more data wearables collect, the better clinicians personalize meal plans. Patients also stay motivated by seeing real-time feedback. A 2022 study found adding wearables to digital records increased user engagement by 32% over 90 days.
Wearables add an invaluable layer of insights for tailored nutrition tracking. Their integration only continues revolutionizing digital health capabilities improving patient care.
This data, combined with standard health records, provides a comprehensive picture. Research shows digital records improve diet coordination by 24%!
Chronic Disease Benefits
Paper logs of what patients eat are now websites and apps. These tools offer new ways to manage lifelong conditions:
- Transform static, outdated data into interactive formats.
- Take quick action as needed
- 87% of doctors find these tools extremely useful for managing diabetes.
- Digital logs empower patients and doctors.
Diabetes Management Case Study
A 2-year digital diet study showed:
- 5% lower key diabetes marker
- 8% better medication adherence
- Faster nutrition consults
Tracking food intake kept patients disciplined. Automated alerts enabled quick responses. Doctors saved time with data analytics.
Personalized Meal Planning

The best part is tailored meal plans. By linking medical needs to diet monitoring, digital systems create customized eating guides. These match foods to an individual’s health markers and tastes perfectly.
Wearable Devices Add Real-Time Insight
Watches, bands, and more collect helpful data:
- Heart rate and activity
- Sleep patterns
- Calories burned
Paired with diet logs, they help calibrate each patient’s nutrition plan. Patients felt 12% more involved with wearable tracking integration. The future will bring even smarter digital diet tools!
Overcoming Key Challenges in Adoption
Despite the immense promise, implementing digital health faces barriers:
- Data Security Concerns: With digital health involving sharing tons of personal patient data, security and privacy risks rise. Using super strong end-to-end encryption, access controls, and patient permission protocols should reduce worries. Responsible data handling that puts people first builds needed trust.
- Getting Doctors and Staff Up To Speed: Many health providers have been slow to fully adopt new digital systems. Providing extensive digital health training programs will highlight the long-term benefits, thereby increasing enthusiasm for the potential of this technology. Starting gradually with support as comfort grows helps smooth the transition period while people learn the systems.
- Making Access More Affordable and Fair: To give wider access to digital health across different economic groups, platforms need to progress beyond expensive wearables toward inclusive and reasonably priced innovations. Significant nationwide investments into healthcare infrastructure and subsidies for connected care are essential to prevent unfair gaps in care.
The Future of Digital Nutrition in Healthcare
As digital health platforms evolve to become more intelligent and comprehensive, they are poised to unlock new possibilities in hyper-personalized, real-time care. With the transformation of smartphones into round-the-clock virtual health assistants and the integration of body scanners in homes, the future is undoubtedly set for a transformative shift. Public policy must establish regulatory foundations and address ethical dilemmas, building trust and transparency.
The journey has only just begun.
FAQs
How can digital health records enable personalized nutrition planning?
By continuously tracking medical vitals and diet metrics, digital records create a multidimensional profile from which personalized meal plans, nutrient recommendations, and portion sizes can be derived based on individual health status.
What policy changes are needed to drive the adoption of digital health in nutritional care?
Governments should build robust digital infrastructure, cybersecurity protocols, and interoperability standards. Incentivizing the digital transformation of independent practices and expanding telehealth reforms will further catalyze adoption.
Bottom Line
Digital health has the potential to drive the next breakthrough in preventive, personalized nutritional care. The management of chronic diseases and patient engagement have already shown significant improvements. As we advance into a future of smarter, proactive, and patient-centric healthcare, overcoming adoption barriers and addressing security and privacy concerns will be crucial.

